RETINOBLASTOMA IN CHILDREN
by Víctor M. Villegas, M.D.
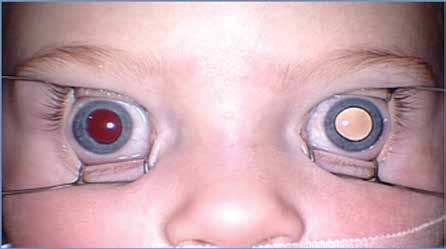
FIGURE 1. CHILD WITH RETINOBLASTOMA IN THE LEFT EYE AND A WHITE PUPIL REFLEX ON FLASH PHOTOGRAPHY.
Retinoblastoma is the most common intraocular malignancy in children. It affects 1 in 15,000 live births. Early diagnosis is of critical importance because small tumors have the best prognosis. Historically, leukocoria or “white pupil” has been the most important sign as seen in Figure 1. It may sometimes be noticed in a photograph taken with flash. Strabismus, nystagmus, red eye, and loss of binocularity can all be presenting signs depending on the location of the tumor.
Therapies for retinoblastoma have dramatically advanced during the last 10 years. A significant trend away from systemic chemotherapy to directly ocular and intra-arterial chemotherapy is currently underway. Technological changes and strategies focus on local treatments due to decreased morbidity to patients and excellent tumor response. New treatments are providing new hope to patients, especially to those with the most severe disease.
Management of retinoblastoma tumors requires a multidisciplinary approach that may include an ocular oncologist, pediatric oncologist, pediatric ophthalmologist, pediatrician, interventional radiologist, and ocular pathologist. Individualized treatment, considering factors such as the International Classification of Retinoblastoma, laterality, location of tumors, age of patient, family
history, and prior treatment must be considered. Retinoblastoma treatment is aimed at child survival.
Globe salvage and preservation of vision are secondary goals. Early diagnosis remains the most crucial step in decreasing morbidity and mortality. Treatment of small tumors may only require transpupillary thermotherapy. Laser treatments may be repeated monthly until complete tumor regression is documented. It is important to follow up patients closely to monitor for recurrence. If recurrence is present, adjuvant chemotherapy may be considered.
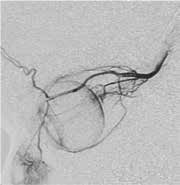
FIGURE 2
New technologies have allowed physicians to improve tumor regression rates while decreasing systemic side effects. Currently, Bascom Palmer Eye Institute is one of the few hospitals in the world that is performing intra-arterial chemotherapy for retinoblastoma. The technique consists of catheterization of the internal carotid artery and the ophthalmic artery with direct infusion of chemotherapeutic agents into the eye vasculature (Figure 2). This technique allows the ocular oncologist to use different chemotherapeutic options and dosing strategies. Direct infusion of chemotherapies to the ophthalmic artery also decreases the systemic side effects experienced by the patient.
The significant tumoricidal effects reported with intra-arterial chemotherapy generated enthusiasm to study intravitreal
delivery for vitreous seeding. During the last three years, Bascom Palmer Eye Institute has been on the forefront in adapting new intravitreal techniques that help control vitreous seeding in patients that would have otherwise lost the eyeglobe. The combination of intra-arterial and intravitreal chemotherapy has allowed us to take care of patients in unprecedented ways. We are extremely excited about the improvements made during the last decade and are looking forward to developing new techniques that improve further the visual outcomes.


Leave a Reply
Want to join the discussion?Feel free to contribute!