Bowlegged Deformity (Genu Varum) and How To Help It
Knee osteoarthritis is one of the leading causes of disability in the United States and it increases with the aging population.

by Paula Allia PT, DHSc, MTC, OCS
The alignment of the leg bones (femur, tibia, and patella) is what determines where joint compressions occurs.
The normal smooth shiny surface (articular cartilage) at the end of bones is where natural rolling and sliding of the bones take place to allow for purposeful movements.
Injuries to the knee joint and muscular imbalances around the joint can lead to deformity of the knee. The progression and type of deformity depends upon the angle of the joint and good muscular balance between flexibility and strength of the surrounding muscles. Without these the biomechanics change and compensatory movements ensue.
In the knee, there is articular cartilage between the thigh bone (femur) and the lower leg bone (tibia) and the kneecap (patella). Normal healthy articular cartilage is smooth and shiny and this aids in smooth gliding and sliding of the bones with movements.
The meniscus is the other type of cartilage and this is wedged on the medial side and lateral (outer side) between the femur and tibia. These menisci allow for the secure positioning between the upper thigh bone and the lower (tibia). If this meniscus is torn, fraying will occur and the joint will eventually become incongruent and cause breakdown that will eventually lead to the deterioration of the articular cartilage.
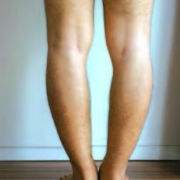
If the medial meniscus is affected, the medial articular cartilage degenerates, compression to this side worsens and the bones angle (genu varum, or bow leggedness).
The weight bearing load shifts more medially and over time causes the lower tibial bone to bow outwards causing this condition.
Gait changes and pain ensues at some point due to the compression and bone pain. The ligament becomes more lax so the stability of the joint gets compromised due to the stresses placed upon it. Pain worsens and can be debilitating. The eventual articular cartilage erosion and decreasing joint stability progresses to bone on bone dysfunction, which leads to more pain.
What can be done to help the joint function better to delay the need for a replacement? First, if you notice that the leg is bowing out and still do not have pain, use a prophylactic approach. Not only should knee alignment be evaluated but also hip and ankle/foot alignment must be considered. The goal is to lessen the laxity of the joint so that abnormal movement patterns do not progress furthering more degenerative joint breakdown.
No treatment to date has ever been able to reverse the degenerative process but recently a study between Harvard and Spalding Rehab discovered a longevity protein called Klotho that decreases with degeneration and this may be a key to helping regenerate the tissue. Currently muscular strength, balance and available range of motion throughout the leg are pertinent to try and realign the knee structures in such a way as to decrease the compression. Many times there are certain tightnesses and weaknesses that coincide with genu varum, so correcting these imbalances before severe progression is key.
Bowleggedness affects stability particularly from side to side and not so much forward and backwards. The gluteus Medius muscle is the biggest supporter of side to side activity and is especially needed in unilateral stance. With progression of the bowed legs, the gluteus Medius needs to be even more strong due to the torque on the leg. In the thigh, the vastus lateralis is weaker and iliopsoas muscles are weaker.
Overall muscular balance is key to minimally slowing down further breakdown of the knee joint Stretching of the hamstrings and the piriformis muscles while working to correct strength imbalances must be considered to help decrease both pain and dysfunction. Keep your knees as healthy as they can be.
Here’s To Your Health!
For further information call Fitness Together in downtown Naple sat 239.263.9348. We have been in business here for 19 years so give us a call today!



Leave a Reply
Want to join the discussion?Feel free to contribute!